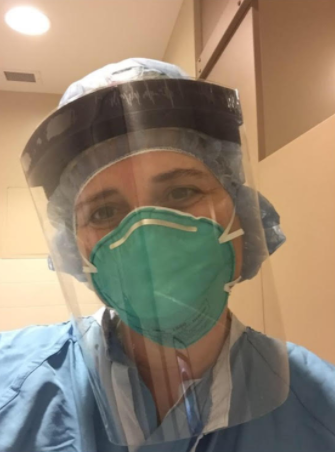
For Niagara Health employees Lisa Laughton and Maria Roberts Ramos, both Niagara-on-the-Lake residents, it was the uncertainty of the early days of the pandemic that caused them much stress back in March and April.
Now, approaching the 10-month mark, they’ve both settled into the routines that have become a way of life in Niagara’s health care system.
Laughton, a registered nurse, works in the recovery room at the St. Catharines site of the Niagara Health System. It’s a position she took on about three years ago, after a number of years in the emergency room.
“It’s really different working in a pandemic,” reflects Laughton. “The biggest thing was the fear of the unknown. In the beginning, we were seeing the media from other countries with mass casualties and strained health care systems. For a lot of us it was fear of the unknown, fear of not enough PPE (personal protective equipment), and fear of having to be separated from my family.”
Though as a nurse, Laughton was already well-trained in infection control measures, she says she very quickly learned new methods that would keep her two high-school aged daughters and her husband Rob, a retired teacher, safe.
“In the beginning, I was coming home, getting undressed outside and going straight into the shower before even talking to anyone in the family,” she says. “At the hospital, we’re all well-versed in infection control. When the hospital administration put policies and plans into place, it wasn’t hard to execute them, and that gave us more confidence and made us all feel a little better.”
As the focus around the world turned to health care professionals and the fight against the novel coronavirus, Laughton and her colleagues circled the wagons in the effort to control the spread. “We’re pretty tenacious,” she tells The Local. “We look at this virus as our enemy, just like the rest of the world. I feel like we’re at battle, and we won’t be beaten. We have a job to do, our patients are number one, and that’s why we go to work every day.”
During the earlier lockdown stages of the pandemic, Niagara Health postponed all elective and non-emergent health care procedures to protect patient safety and increase capacity for the response to COVID-19. That meant for the most part things were a bit slower in the recovery room where Laughton works. She credits Niagara Health for making wise decisions, which enabled local hospitals to reserve the capacity to take on coronavirus patients in the intensive care unit.
Now, with the volume closer to normal on the elective surgery front, the hospital is working through the list as quickly as they can. “We’ve learned since the spring, we’ve tweaked things, and at the same time we’re ready for the second wave,” Laughton explains.
She feels the decision by Premier Doug Ford to move Ontario into the grey zone on Dec. 26 was the correct one, in light of the high COVID-19 numbers recently. “We needed to do that,” Laughton confirms. “I think we all let our guard down in the summer, but it’s winter time, and we’ve moved inside. I’m confident that we’ll keep plugging away, a vaccine will soon be distributed, and that things will improve if we keep doing what we’re doing.”
She credits the teams at Niagara Health who put policies in place for alleviating those early fears of the unknown that she and her colleagues had. “I’m positive about the organization, and how we’ve all pulled together. We feel confident in what we’re doing, and we’re all supportive of each other, whether I work with you in my inner circle, or in the hospital as a whole. You can just tell that we’re there for each other. We feel like this virus is the enemy, and we’re at battle. It’s not going to stop us from doing what we do.”
Though Laughton says the praise that has been heaped onto health care workers since March makes her proud of her role as a nurse, she deflects some of that praise onto others in the community. “We’re all in this together. I feel like we’re all in the front lines. If we don’t all do what we need to do, then we’re not going to have the best outcome. We all have to work together to do this, not just the health care professionals.”
Similarly for Maria Roberts Ramos, a speech language pathologist, the stress of the unknown at the onset of the pandemic has been replaced by a confidence that upgraded infection control methods and procedures are effectively allowing her to continue in her role in the health care system.
Though Roberts Ramos is employed by Niagara Health, her position is overseen by the Niagara Preschool Speech and Language Program through the Niagara Children’s Centre. Her office is attached to the Greater Niagara General site in Niagara Falls, though she doesn’t actually have to enter the hospital building itself.
Like Laughton, her job was never interrupted during the first wave of the outbreak, though there were some changes to how she delivered service to families.
Before COVID-19, Roberts Ramos would arrive at her office at 8:30 a.m. Throughout each day she would work with between four and five families, helping children, with an average age of two years old, with early speech development. This involves face-to-face meetings with the children and their families, working on communication strategies for those who have been assessed as experiencing difficulties in language and communication development.

Like many in the health care system, she was ready for any changes to her role, including being shifted to other duties to support the overall goals of Niagara Health if necessary. “We were told we might be moved, but because we were always able to maintain contact with our families and continue offering service, we weren’t.”
For the first two to three months of the pandemic, Roberts Ramos shifted to telephone consultations with her client families. “I’ve been going into the office all through this,” she says. “I would call families, ask how things were going, the parents and I would talk. We would problem-solve, I would give them suggestions through these phone conversations.”
She admits she worried somewhat that some of her client families would not be able to receive the guided help with communication strategies that they would have via her usual routine. “When you think health care, you think of hospitals and surgeries,” she says. “But parents who had had an assessment would have to wait a much longer time to get the help they needed. That’s the impact of COVID that a lot of people don’t think about. Kids need rehab. We did the best that we could, but there was some impact on the ability of some children to move forward with their development and connections to other resources.”
Over that early stage of the pandemic, Roberts Ramos and her colleagues were able to learn new techniques to move into a virtual method of delivering services to families via Zoom Health, a more secure form of the Zoom platform used by health care professionals.
“It’s new to us, but it’s not new to the profession,” explains Roberts Ramos. “Up north, where people can’t travel, this is how they provide therapy. Our focus shifted early on to developing materials and learning ourselves how to do virtual therapy online with preschoolers.”
She has clearly enjoyed learning the new techniques, and felt very supported by both Niagara Health and the Children’s Centre in developing new methods. She even sees some advantages to the virtual platform for continued future use.
“You get to see the children in their home environment,” she enthuses. “You can talk to the parents and say ‘show me what that looks like in your kitchen,’ you can coach them right online on how to get through to the child. Or they have siblings, who want to be in on it, so you can include them right there.”
Now, more than nine months in, Roberts Ramos is back in her office and has been seeing clients for face-to-face sessions since early fall, while still offering virtual options as well. Though a COVID-19 outbreak was declared at the Niagara Falls site on Dec. 24, she is not worried about working out of her office.
“I’m not right in the hospital,” she says, “and when we started seeing families in person again, NHS was really good with providing screens, masks, goggles, face shields, gloves, everything we needed to feel protected. There’s a screener downstairs as well, and we disinfect toys, tables, chairs, doorknobs and all touch points. And I’m not dealing with sick people in my role.”
As Roberts Ramos heads back to work Jan. 4, she has yet to hear if the province’s month-long lockdown will allow her to continue with those face-to-face sessions. But she is optimistic.
“The hospital is trying very hard to maintain their outpatient services,” says Roberts Ramos. “We do have protocols now, we know how to keep people safe. They understand how important services are. I think everybody recognizes the importance of keeping these services available.”